Scientific Calendar December 2018
What is the clinical value of knowing the CD4 count of an HIV-infected individual?
It is used as a guide to know when to discontinue antiretroviral therapy
It is used to confirm the diagnosis of opportunistic infections
It is used to identify individuals with advanced HIV disease who would benefit from intensified support – the lower the count the greater the risk of illness and death
It is used to assess the rate of HIV replication and risk of onward transmission
Congratulations!
That's the correct answer!
Sorry! That´s not completely correct!
Please try again
Sorry! That's not the correct answer!
Please try again
Notice
Please select at least one answer
Scientific Background
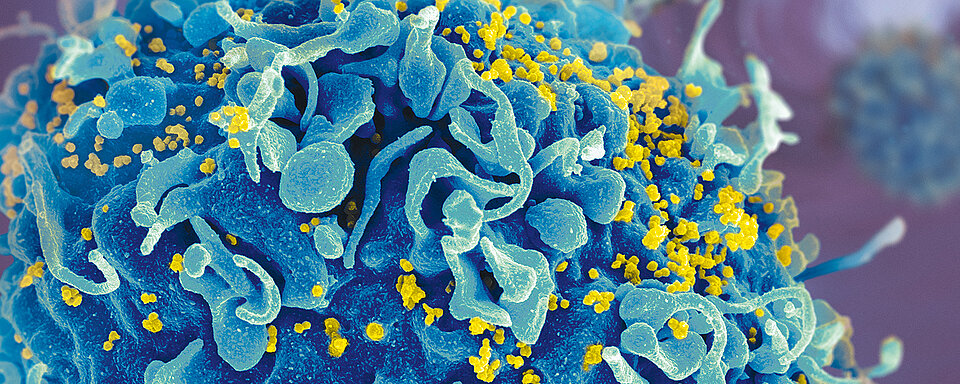
The pathogenic mechanisms of human immunodeficiency virus (HIV) infection are complex. HIV primarily targets CD4+ T cells, attaching itself to the surface and gaining entry into the cell where it starts to multiply. In the early stages of infection, viral replication is prominent resulting in rapid and extensive depletion of CD4+ T cells. This leads to massive viraemia and widespread dissemination to all lymphoid tissues of the body. By the time an individual has developed antibodies to the virus and tests positive for HIV with conventional serology tests, the infection is already well-established. The body produces billions of new CD4+ cells to replace those that have been destroyed. If left untreated, infection with HIV will result in the progressive deterioration of the immune system, breaking down the body’s ability to fight off infections and other diseases. Acquired immune deficiency syndrome (AIDS) refers to the most advanced stages of HIV infection, defined by the occurrence of any of several opportunistic infections or related cancers.
As ongoing viral replication is directly linked to progressive loss of CD4+ cells in both function and number, the mainstay of treatment is to disrupt the viral lifecycle. A vast body of research data has identified that effective viral suppression requires the use of a cocktail of drugs, collectively referred to as antiretrovirals (ARVs), the name reflecting the family Retroviridae to which HIV belongs. As these drugs and the tests needed to monitor patients on antiretroviral therapy (ART) were initially prohibitively expensive for wide scale implementation, treatment was originally reserved for individuals with advanced immunosuppression. The World Health Organization (WHO) developed comprehensive guidelines on how to determine who was eligible for enrolment into ART programmes. Although other clinical factors were considered, the primary criterion of such selection was the CD4 count, as it is the most important laboratory indicator of immune function in HIV infected individuals. A combination of a reduction in costs of both drugs and laboratory tests, based on economies of scale of mass production, and an increased global commitment to fighting HIV with concomitant increase in funding has led to the adoption of the “test and treat” principle, whereby ART should be initiated for all at the time of diagnosis of HIV infection, irrespective of CD4 count. Also, as HIV viral load (HIVVL) testing has become more affordable and accessible, HIVVL rather than CD4 count is preferred to monitor response to ART.
Although the CD4 count is no longer essential for treatment initiation, and HIVVL is the preferred monitoring test to assess viral suppression, it remains a critically important test in the management of HIV disease.
So, when should a CD4 test be done and why?
When HIV is first diagnosed.1
This is not to determine if treatment should be started, but rather to have a baseline value for reference should the individual develop complications in the future (ART must be taken lifelong). Also, many patients already have advanced disease at the time of diagnosis and may benefit from prophylactic antibiotics to prevent opportunistic infections.
When restarting ART after a break in treatment.1
This is to establish a new baseline and to see if there has been any progression in disease due to the period of non-adherence to treatment.
When a person is ill and there is a clinical suspicion of advanced HIV disease.1
Advanced HIV disease carries a high risk of death; hence it is important to identify such individuals so that they can benefit from an intensive package of supportive care.2 The CD4 counts guide the need for additional testing and support for associated opportunistic infections (e.g. TB, cryptococcal meningitis and toxoplasmosis).3
When there is evidence of treatment failure (VL >1000 copies/ml twice in a row).1,3
Failure of viral suppression puts the individual at risk of worsening immune suppression, due to ongoing depletion of CD4+ T cells. Such individuals may be at risk of advanced disease and will require a switch of treatment regimen if non-adherence is excluded as a cause of treatment failure.
To monitor response to treatment if HIVVL testing is not available.1
Although HIVVL is the preferred test to assess viral suppression, the CD4 count is useful as a surrogate marker, as failure of suppression would ultimately manifest with declining CD4 counts.
References
- Guidelines for managing advanced HIV disease and rapid initiation of antiretroviral therapy. Geneva: World Health Organization; July 2017.
- What's new in treatment monitoring: viral load and CD4 testing. Geneva: World Health Organization; July 2017
- Waiting isn't an option: preventing and surviving advanced HIV. Medecins Sans Frontiers; July 2017